Rethinking Meniscus Surgery: What a Landmark Trial Means for Knee Pain Management
Overview
For decades, arthroscopic partial meniscectomy—shaving off a torn piece of knee cartilage—was one of the most common orthopedic procedures worldwide. Surgeons believed that removing the damaged meniscus would relieve pain and improve function. However, a major 10-year clinical trial has upended this belief. The study found that the surgery offers no real benefit over a placebo (sham) operation and may actually worsen long‑term outcomes, including more symptoms, poorer function, faster progression of osteoarthritis, and a higher chance of needing additional surgery. This guide explains the trial’s design, key findings, and what they mean for patients and healthcare providers.
Prerequisites
- Basic understanding of knee anatomy (meniscus, cartilage, joint function)
- Familiarity with common knee injuries (e.g., meniscal tears)
- Some knowledge of clinical trial concepts (placebo, randomization, sham surgery)
- Optional: access to online medical databases for further reading
Step‑by‑Step Guide: Understanding the Trial and Its Implications
1. The Meniscus: Function and Tears
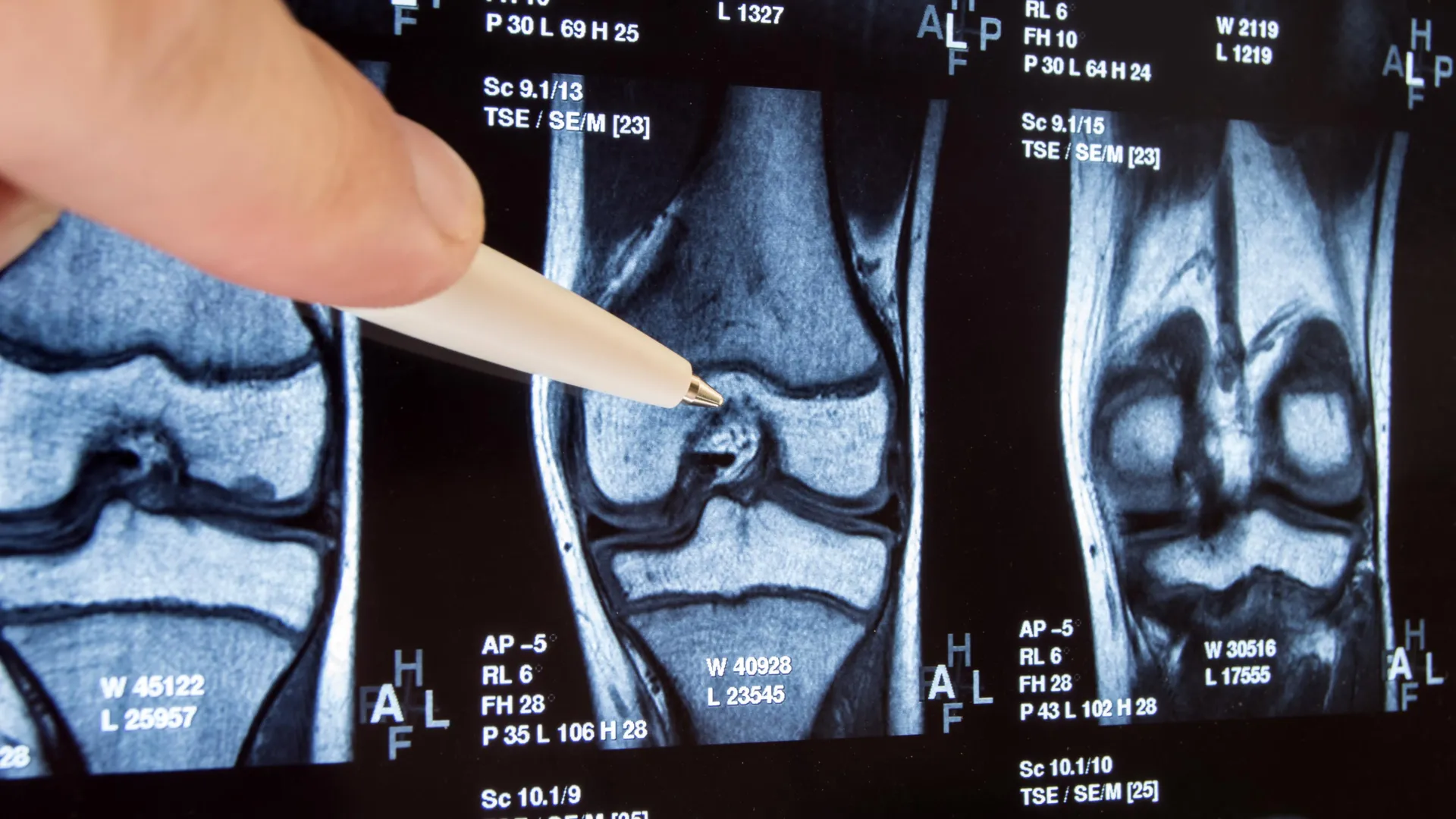
The meniscus is a C-shaped piece of cartilage that acts as a shock absorber and stabilizer in the knee joint. Tears can occur from trauma or degenerative wear. A torn meniscus often causes pain, swelling, and limited motion. Traditionally, surgeons recommended trimming the torn part (partial meniscectomy) to eliminate mechanical irritation.
2. Why This Surgery Was So Common
Partial meniscectomy gained popularity because it is minimally invasive, has a short recovery time, and many patients reported immediate pain relief. However, those reports were based on uncontrolled observations—patients expected to improve, and surgeons attributed any benefit to the procedure itself. The placebo effect was not properly accounted for.
3. The Landmark Clinical Trial Design
The Finnish Degenerative Meniscal Lesion Study (FIDELITY) randomized 146 patients with a degenerative medial meniscus tear to either arthroscopic partial meniscectomy or sham surgery (a skin incision and scope insertion but no trimming). Neither patients nor outcome assessors knew which group they were in. Follow-up continued for 10 years.
4. Key Findings Over 10 Years
- No difference in pain relief: Both groups reported similar reductions in knee pain at all time points.
- Worse symptoms in the surgery group: Patients who had the real surgery reported more pain, stiffness, and difficulty with daily activities over the long term.
- Poorer function: Objective measures like walking speed and strength were inferior in the surgery group.
- Faster osteoarthritis progression: Radiographic evidence showed that joint space narrowing (a sign of arthritis) accelerated in the surgical group by about 40% compared to placebo.
- Higher reoperation rate: Patients who received the real surgery were nearly twice as likely to undergo a second knee procedure (e.g., knee replacement) within 10 years.
5. Implications for Clinical Practice
These results challenge the routine use of partial meniscectomy for degenerative tears. The American Academy of Orthopaedic Surgeons now recommends against the procedure for most patients with knee osteoarthritis. Instead, conservative management—physical therapy, anti‑inflammatory medications, activity modification—should be the first line of treatment.
6. What This Means for Patients Considering Surgery
- Discuss the possibility of a placebo response with your surgeon.
- Ask about high‑quality rehabilitation programs before opting for an arthroscopy.
- Understand that removing meniscus tissue may hasten arthritis.
- Consider second opinions from specialists who are aware of this trial.
Common Mistakes
- Mistaking correlation for causation: Early improvement after surgery is often due to natural healing or the placebo effect, not the trimming itself.
- Ignoring long‑term data: Short‑term satisfaction (e.g., 6 months) can mask progressive joint damage that becomes evident only after years.
- Overgeneralizing to traumatic tears: This trial studied degenerative tears in older adults (average age 52). Younger patients with acute, traumatic tears may still benefit from partial meniscectomy—more research is needed.
- Skipping conservative care: Many patients try surgery before exhausting non‑surgical options like physical therapy, which has been shown to equal the short‑term outcomes of surgery with fewer long‑term risks.
Summary
A decade‑long randomized trial has demonstrated that arthroscopic partial meniscectomy for degenerative meniscal tears offers no benefit over placebo and may accelerate osteoarthritis and lead to worse function over time. This evidence calls for a paradigm shift in knee pain management: prioritize conservative treatments and critically evaluate the role of surgery. Patients and clinicians should engage in shared decision‑making that incorporates these long‑term outcomes.